If there’s one thing life teaches you, it’s that some problems are too embarrassing to discuss—until they’re your problem. Hemorrhoids are like that annoying neighbor who doesn’t knock before entering your house. One day, you’re living your best life, and the next, you’re waddling around like a penguin, wondering if you’ll ever sit comfortably again. But let’s cut through the nonsense. The medical world wants you to believe that hemorrhoids are caused by a lack of fiber and whole grains.
That’s like saying a lack of traffic lights causes car crashes—a convenient lie that sells solutions while ignoring the root cause. So, what really causes hemorrhoids? And more importantly, how do you prevent them without shoveling down a mountain of indigestible plant material? Buckle up, Tribal Chief. We’re about to break it down like a butcher carving up a fresh slab of nyama choma.
What Are Hemorrhoids?
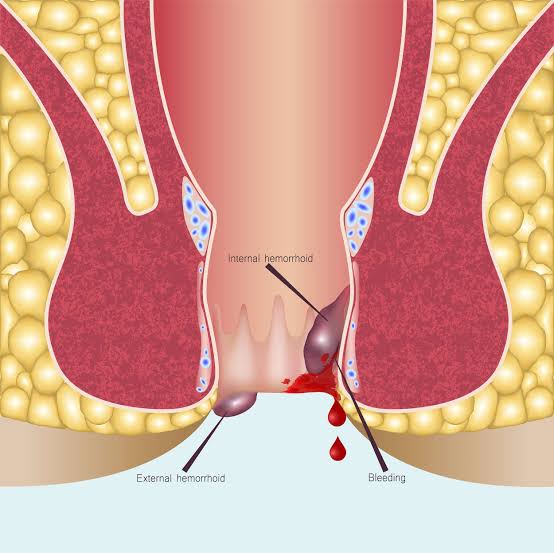
Hemorrhoids, also known as piles, are swollen veins in the anus or lower rectum.
Think of them as varicose veins, but instead of being on your grandma’s legs, they’re in the worst place possible—your backside.
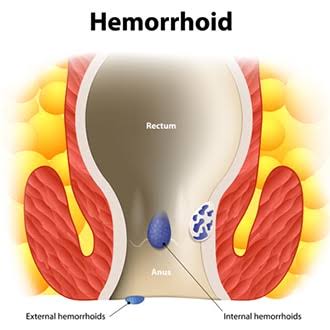
There are two main types:
- Internal Hemorrhoids – These hide inside your rectum like cowards. You usually don’t feel them unless they decide to bleed or prolapse (peek outside like a curious groundhog).
- External Hemorrhoids – These are right under the skin around your anus, where they can swell, itch, and hurt like hell.
If they develop a blood clot (thrombosed hemorrhoid), you’ll know pain on a deep spiritual level.
Basically, hemorrhoids are what happens when the delicate veins in your backside get overworked and swollen.
They’re like a rubber band stretched too much—eventually, something’s gotta give.
Now, what causes this mess?
Forget the “eat more fiber” fairy tale—that’s just Big Grain selling you overpriced sawdust.
The real causes of hemorrhoids boil down to pressure, poor circulation, and inflammation. Let’s break it down:
- Straining on the Toilet (a.k.a. The Birth of a Hemorrhoid)
If you’re pushing like you’re trying to deliver a baby elephant, you’re asking for trouble.
Straining increases pressure in the rectal veins, making them swell and bulge.

Why do people strain?
Eating processed junk that slows digestion.
Ignoring nature’s call and letting stool harden like cement.
Sitting too long on the toilet, scrolling through social media instead of handling business efficiently.
- Sitting Too Much (a.k.a. The Desk Job Curse)
Sitting for long hours, especially on hard surfaces, crushes your blood flow down there.
It’s like putting your foot on a garden hose—eventually, pressure builds, and veins swell.
- Weak Connective Tissue (a.k.a. The “Grandpa Problem”)
As you age, your tissues lose elasticity, making it easier for veins to stretch and sag.
Think of an old pair of socks—they don’t hug your legs like they used to.
- Chronic Inflammation (a.k.a. The Real Enemy)
Inflammation weakens blood vessels and makes them more prone to swelling. What causes this?
High-carb, grain-based diets (especially seed oils and processed sugars).
Alcohol and excessive caffeine, which dehydrate you and make stool harder.
Gut dysbiosis—an unhealthy gut means bad digestion, bloating, and pressure in all the wrong places.
- Pregnancy (a.k.a. The Baby is Sitting on Your Veins)
For women, pregnancy is a hemorrhoid factory.
The weight of the baby presses on veins, and hormonal changes make tissues softer.
Combine that with pregnancy constipation, and it’s a perfect storm for hemorrhoids.
- Lifting Heavy with Bad Technique (a.k.a. The Gym Bro Problem)
If you hold your breath and push too hard when deadlifting, squatting, or doing strongman-style lifts, you’re spiking intra-abdominal pressure.
This can pop out a hemorrhoid faster than a faulty champagne cork.

Predisposing Factors for Hemorrhoids
Some people are just more prone to hemorrhoids than others.
It’s like how some guys can eat anything and stay lean, while others look at a plate of ugali and gain 5kg.
Here’s what puts you at higher risk:
- Genetics (a.k.a. “Thanks, Mom and Dad”)
If your family has a history of weak veins or varicose veins, you’re already playing on hard mode.
Some people inherit weaker connective tissues, making their rectal veins more likely to swell and bulge.
- Chronic Constipation or Diarrhea
Constipation = You push too hard, building insane pressure in your rectum.
Diarrhea = Frequent wiping and irritation cause inflammation and weakening of veins.
Either way, your anus is taking damage.
- Sedentary Lifestyle (a.k.a. “Sitting Disease”)
Sitting too much crushes circulation down there.
Lack of movement makes digestion sluggish, leading to constipation.
Your veins get weaker over time because they don’t get enough blood flow.
- Low-Fat, High-Fiber Diets (a.k.a. The Rabbit Food Problem)
The mainstream advice is a scam. Too much fiber can:
Bulk up stool too much, making you strain.
Cause bloating and gas, adding more pressure to your gut.
Ferment in your intestines, leading to irritation and inflammation.
- Dehydration (a.k.a. The Dry Gut Disaster)
Not drinking enough water hardens stool, making it painful to pass.
Too much caffeine and alcohol can make it worse by dehydrating you.
If your electrolytes are off (low sodium, potassium, or magnesium), your intestines won’t function properly.
- Obesity (a.k.a. “Extra Weight, Extra Pressure”)
Excess body fat, especially around the abdomen, increases pressure on the pelvic veins.
This slows blood flow and creates a perfect storm for hemorrhoids.
- Pregnancy (for Women)
We covered this before, but in short:
The baby is pressing on veins like a weightlifter.
Hormones soften tissues, making hemorrhoids more likely.
Constipation during pregnancy makes things worse.
- Heavy Lifting with Poor Breathing
If you hold your breath and strain too much while lifting, you force blood into your rectal veins, increasing pressure and making hemorrhoids more likely.
Proper breathing (like the Valsalva maneuver with control) helps avoid this.
Pathophysiology of Hemorrhoids (a.k.a. How Your Butt Veins Betray You)
Hemorrhoids develop when the veins in your anal and rectal region become swollen, inflamed, and weakened due to excessive pressure or poor blood flow.
Step-by-Step Breakdown of the Hemorrhoid Disaster
- Increased Venous Pressure = Vein Swelling
The superior, middle, and inferior hemorrhoidal veins drain blood from your rectum and anus.
When there’s excessive pressure (from straining, prolonged sitting, or pregnancy), these veins get engorged with blood because the blood can’t flow back efficiently.
This leads to vein dilation and swelling, forming hemorrhoidal cushions (the start of hemorrhoids).
- Weakened Connective Tissue = Loss of Support
Normally, the rectal veins are supported by strong connective tissue that keeps them in place.
Over time, due to aging, inflammation, and poor diet, these tissues lose elasticity and weaken.
The swollen veins start sagging and protruding into the rectal canal or out of the anus.
- Inflammation & Irritation = Pain, Bleeding, and Itching
The constant swelling and irritation cause inflammation, which leads to pain and itching.
If the veins become stretched too much, they rupture and bleed (leading to bright red blood in stool).
If external hemorrhoids develop blood clots (thrombosis), they become hard, painful lumps that can make sitting unbearable.
- Chronic Damage = Prolapse & Complications
In severe cases, internal hemorrhoids prolapse, meaning they fall out of the rectum and hang outside the anus.
If they get stuck outside for too long, they can become strangulated, cutting off their blood supply and leading to necrosis (tissue death).
The Simple Version (for Non-Doctors)

Imagine your rectal veins are like small balloons.
Normally, blood flows in and out freely.
But if you apply too much pressure (straining, sitting too long, lifting heavy) or weaken the support structure (bad diet, aging, inflammation),
those balloons swell up and get stuck.
If they get too big, they start hanging out where they shouldn’t.
If they rupture, they bleed. If a clot forms, they hurt like hell.
Signs, Symptoms, and Diagnosis of Hemorrhoids (a.k.a. How to Tell if Your Butt’s Been Betrayed)
Hemorrhoids aren’t just an inconvenience; they’re an in-your-face problem that leaves you with a literal pain in the ass.
Let’s break down how to spot them, what you might feel, and how doctors diagnose the situation.
Signs and Symptoms of Hemorrhoids (a.k.a. The Red Flags)
- Bleeding (a.k.a. The “Oh No, Not Again” Moment)
The most obvious and terrifying sign of hemorrhoids is bright red blood on your stool, toilet paper, or in the toilet bowl.
But here’s the kicker: It’s usually not as serious as it looks.
Hemorrhoid bleeding is generally painless and occurs because the swollen veins rupture when you pass stool.
What it looks like: Bright red blood, often in small amounts.
Why it happens: The swollen hemorrhoidal veins in the rectum burst under pressure.
- Itching and Irritation (a.k.a. The Itch from Hell)
The itch is real, and if you’ve ever had hemorrhoids, you know the feeling.
The anal area can get itchy and irritated, especially if you’ve been wiping too much or dealing with inflammation.
What it feels like: A persistent, annoying itch that won’t go away.
Why it happens: Swelling and inflammation irritate the skin around the anus.
- Pain and Discomfort (a.k.a. Sitting Becomes a Mission)
If the hemorrhoids are external, they can become painful, especially when sitting, standing, or walking.
If a clot forms (a thrombosed hemorrhoid), it can feel like a hard, painful lump.
What it feels like: A sharp pain or throbbing when sitting, especially on hard surfaces.
Why it happens: Swollen veins become irritated, and blood clots may form, causing intense pain.
- Swelling or Lumps (a.k.a. The “Bubble Butt” Look)
When hemorrhoids become external, you might feel or see swollen lumps near the anus.
These lumps may be soft or hard, depending on whether they are thrombosed or not.
What it feels like: A swollen, sometimes painful lump near your anus.
Why it happens: The veins around the anus swell and protrude, sometimes forming a clot.
- Prolapse (a.k.a. When Your Butt Speaks Up)
Internal hemorrhoids can prolapse, meaning they fall out of the anus when straining or after a bowel movement.
You may have to push them back in manually.
What it feels like: A bulge that sticks out of your anus, especially during bowel movements.
Why it happens: When internal hemorrhoids swell and lose support, they prolapse and hang outside.
- Mucus Discharge (a.k.a. TMI, but Necessary)
Some people experience a mucus discharge from the anus.
This is less common but happens when hemorrhoids cause irritation or inflammation.
What it feels like: A slippery, sometimes uncomfortable feeling or spotting mucus.
Why it happens: The irritation from hemorrhoids stimulates mucus production.
How Hemorrhoids Are Diagnosed (a.k.a. What Your Doctor Does When You Finally Go in for Help)
If you’ve got bleeding, pain, and swelling, don’t wait for it to magically go away.
Hemorrhoids need to be officially diagnosed to rule out more serious conditions (like cancer).
Here’s what your doctor will likely do to confirm it’s hemorrhoids:
- Physical Examination (a.k.a. The “Bend Over and Cough” Part)
The doctor will examine the anal region to check for external hemorrhoids (those lumps you can feel).
For internal hemorrhoids, they may use a gloved finger to feel for abnormalities.
- Digital Rectal Exam (DRE) (a.k.a. The Finger Check)
The doctor will insert a gloved finger into your rectum to feel for abnormalities such as internal hemorrhoids or lumps.
This might sound awkward, but it’s necessary to feel for any internal swelling, tenderness, or prolapse.
- Anoscopy (a.k.a. The Tube Investigation)
For a more thorough examination, your doctor may use an anoscope—a small, rigid tube with a light at the end—to get a closer look at the inside of your rectum.
This allows them to assess the severity of internal hemorrhoids and check for other potential issues, like infections or tumors.
- Sigmoidoscopy/Colonoscopy (a.k.a. When They Want to Rule Out Cancer)
If you’re over 50 or have a family history of colon cancer, your doctor may recommend a sigmoidoscopy or colonoscopy to ensure there’s nothing more serious going on.
This is a more invasive procedure where a flexible tube is used to examine the colon and rectum for abnormalities like tumors or polyps.
If you notice bleeding, pain, swelling, or discomfort, don’t panic—it’s probably hemorrhoids, but get it checked out to be sure.
Most hemorrhoid symptoms can be diagnosed with a simple physical exam or anoscopy.
Your doctor will rule out anything more serious, like colorectal cancer, before recommending treatment.
Prevention and How to Fix Hemorrhoids (Without Fiber, Promise)
Now, let’s hit the real meat of the matter.
Preventing and fixing hemorrhoids isn’t about shoveling down plant matter or relying on over-the-counter creams.

It’s about getting smart, adjusting your habits, and using natural methods to restore balance.
- Stop Straining (a.k.a. No More Push-Ups in the Bathroom)
You don’t need to strain like you’re giving birth to a baby giraffe.
Straining creates pressure in your rectal veins, and that’s the quickest way to make hemorrhoids.
Listen to your body and don’t hold it in. If you need to go, go! (To the toilet)
If you’re constipated, take steps to soften stool naturally (don’t just bulk it up with fiber). Search our topic on constipation.
Avoid sitting on the toilet for long periods—no social media browsing while on the throne. It’s not a luxury lounge.
- Get Moving (a.k.a. Sit Less, Move More)
A sedentary lifestyle crushes circulation and makes everything sluggish, including digestion.
If you’re sitting all day at work, get up every 30 minutes and walk around or stretch.
Exercise regularly—squats, deadlifts, and other big lifts help with circulation and bowel movements.
Walking is a simple and effective way to improve blood flow and prevent hemorrhoids.
- Adjust Your Diet (a.k.a. Don’t Rely on Fiber as the Magic Bullet)
Here’s where I break it to you: fiber isn’t the hero here.
The problem isn’t that you’re not eating enough plants, it’s that you’re eating the wrong foods.

Eat enough fat—Fat, from animal sources, helps keep things moving smoothly.
Avoid processed foods that cause inflammation, like vegetable oils, sugary snacks, and grains.
Drink enough water! Dehydration hardens stool, and a dry stool is a hemorrhoid’s best friend.
- Use Proper Technique (a.k.a. Don’t Kill Your Gut)
When lifting, be mindful of how you breathe.
Holding your breath and straining will increase pressure in your abdominal cavity and push blood to your rectal veins.
Exhale forcefully while lifting (instead of holding your breath).
Engage your core properly to avoid putting unnecessary pressure on your veins.
- Avoid Prolonged Sitting (a.k.a. The Ass-Crack Death Trap)
Whether it’s a hard chair at work or a long car ride, sitting for long periods adds pressure to your rectal veins.
Take frequent breaks and move your legs around every hour.
Consider using a standing desk or a cushion if you have to sit for long periods.
- Address Underlying Health Issues (a.k.a. Fix Your Gut)
If you have gut dysbiosis or chronic constipation, it’s time to fix that first.
A damaged gut will make everything worse.
Support digestion with bone broth, fermented foods, and low-carb animal foods.
Gut health is key to preventing bloating and constipation, which will cause straining.
- Try Natural Remedies (a.k.a. No Chemical Crap)
Instead of running to the drug store for creams and ointments, try these natural fixes to soothe the area:
Warm sitz baths—Fill a basin with warm salted water and soak your bottom for 15 minutes to reduce swelling and pain.
Witch hazel—Apply some to the affected area. It’s an anti-inflammatory, and it’ll help reduce irritation.
Ice packs—Apply for 10-15 minutes to reduce swelling if you have external hemorrhoids.
- Medical Intervention (a.k.a. If All Else Fails)
In extreme cases where hemorrhoids don’t improve with lifestyle changes or are causing intense pain, you may need to consider more aggressive treatments:
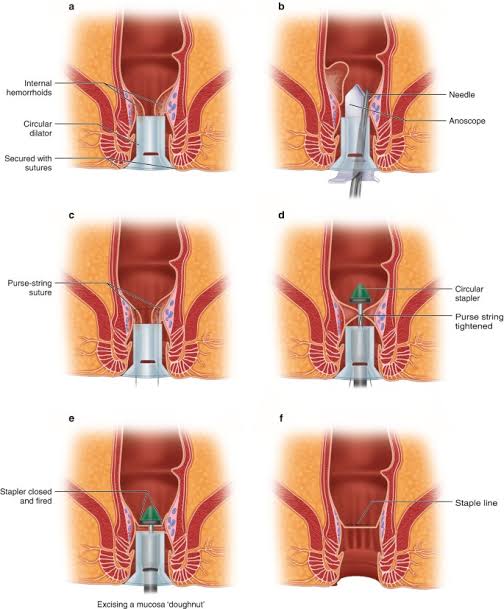
Rubber band ligation—A procedure where a rubber band is placed around the hemorrhoid to cut off its blood supply.
Sclerotherapy—An injection that causes the hemorrhoid to shrink.
Surgical removal—When hemorrhoids are massive and prolapsed, surgery may be necessary.
Prevention and treatment of hemorrhoids are simple but direct.
Focus on healthy, whole foods (not fiber-optic led processed junk), stay active, and avoid prolonged pressure.
If hemorrhoids do show up, natural methods like sitz baths, witch hazel, and healthy fats can help.
If things get really bad, talk to a doctor about options, but always keep your diet and lifestyle in check to avoid future flare-ups.
And remember—don’t trust the fiber hype. Your gut is stronger than they want you to believe.

In conclusion,
Hemorrhoids are a common, yet often embarrassing issue that can cause a lot of discomfort, but they are not the end of the world.
With the right lifestyle adjustments—like avoiding strain, staying active, and eating smart (good fats over fiber bulks),
you can prevent and even manage hemorrhoids without relying on the usual grain-based “solutions” that the food industry pushes.
In the unfortunate event that you develop hemorrhoids, stay calm.
Bleeding and pain don’t automatically signal something deadly.
Most hemorrhoids can be managed with natural remedies like warm baths and witch hazel, and they usually resolve on their own if you adjust your habits.
However, if symptoms worsen or become chronic, getting a diagnosis is essential to rule out more serious conditions and ensure the most effective treatment plan.
Remember, don’t ignore the signs—the sooner you address hemorrhoids, the less likely they are to turn into a bigger problem.
At the end of the day, hemorrhoids are just a part of life for some of us, but with the right knowledge and care, they don’t need to control your life or your bottom.
Stay smart, stay active, and keep that butt happy.

